Preserving pulp in immature teeth: Why is it so important for dentists? by Juan F. Yepes
Preserving pulp in immature teeth: Why is it so important for dentists? by Juan F. Yepes
Dental decay: An overview
Dental decay is the most common chronic childhood disease. Worldwide, 42% of children between the ages of 2 to 11 years old have dental caries in the primary dentition. Premature primary or permanent tooth loss can be caused by dental caries and infection, trauma, or ectopic eruption of permanent teeth, however dental decay is the most prominent cause especially for primary and permanent molars. Poor dietary habits, poor oral hygiene habits, and low socioeconomic status have been shown to be correlated with higher caries incidence and premature tooth loss. Following dental decay as the most common cause of premature loss of primary and permanent teeth is trauma.
Risks of premature tooth loss
Keeping immature (and mature) teeth in the oral cavity is critical for many reasons. Let’s review some of the reasons. Pediatric oral health care has several special considerations within the treatment planning process, including children’s growth and development. Maintenance of arch integrity as children transition from primary to mixed dentition is essential to the development of permanent dentition. The primary dentition has several purposes. Not only does it allow for mastication for adequate nutrition, proper occlusion and esthetics, but they affect the development of speech in children. When lost prematurely, there can be negative consequences seen in the psychological and emotional well-being of children and adolescents. Tooth loss can be considered premature when primary teeth are extracted prior to the normal exfoliation timing. Another major consequence of premature loss of primary teeth is space loss in the permanent arch, as well as crowding and malocclusion. Specifically, the premature loss of primary molars has been found to be associated with major malalignment of the permanent teeth. These effects on succedaneous teeth can result in more expensive and extensive treatment needs in the future.
How to evaluate space maintenance?
Premature tooth loss can lead to space loss but there are several factors to consider when deciding to implement space maintenance for patients in primary and mixed dentition. Specific criteria to consider when evaluating the need for space maintenance includes:
✓ The time that has passed since tooth loss
✓ The chronological age of the child, the dental age or development of the child
✓ Amount of space closure already observed, where in the arch tooth loss is observed
✓ Direction of space closure
✓ The timing of eruption of the succedaneous teeth
✓ The amount of bone remaining over the unerupted permanent tooth.
Premature loss of primary molars poses a significant risk for space loss in the dental arch, making patients three times more likely to require orthodontic treatment after reaching complete permanent dentition. Premature loss of primary anterior teeth does not pose the same risk for space loss in the dental arch. However, premature loss of immature permanent maxillary teeth has deep impact in the esthetics and self-esteem of the patient.
Preserving pulp in traumatized teeth
The occurrence of trauma in the permanent immature teeth is common worldwide. Two thirds of all dental trauma have been reported to occur in children and adolescents with the anterior permanent teeth being the most affected. Traumatic injuries may result in pulp exposure, which may lead to infection. Complicated crown fractures in immature teeth presents a special challenge for the dentist. The main idea is to preserve the pulp inside the root to allow the tooth to complete the root formation and the apex closure. The main objective when preserving the pulp is the use a highly biocompatible material. A favorable material will ensure long term survival of the tooth and avoid the extraction. Various dental materials have advocated for use in direct contact with the pulp.
Traumatized teeth management with Biomaterials
Biodentine™ has excellent properties that protect the vitality of the traumatized tooth pulp:
✓ The setting time, which is around 9-12 minutes. There is a significant difference in the setting time compared with other similar cements (like MTA).
✓ The compression strength of Biodentine™ is similar to the dentin. The use of etch over Biodentine™ does not affect the compressive strength of the material.
✓ The porosity: Because of the low content of water of Biodentine™ the porosity of the material is lower compared with other materials. This is a significant benefit when a perfect seal is mandatory, like in direct pulp cap treatment.
✓ The radiopacity, thanks to the content of zirconium is ideal and allows the practitioner to visualize the material on the radiographs.
✓ The antibacterial property is attributed to the high pH of the material. The high alkalinity has inhibitory effect on the growth of microorganisms.
✓ The biocompatibility of Biodentine™ is outstanding and has been probed in multiple studies when the material is placed with fibroblasts from the pulp.
Preserving immature primary and permanent teeth is a critical task of contemporary dentistry. Placing a dental material in direct or indirect contact with the pulp is a common option that the dentist has in the treatment armamentarium to guarantee the preservation of the pulp tissue. Biodentine™, as described above, is highly biocompatible. This ability was investigated in multiple studies in the past 5 years. Biodentine™, when applied to human pulp cells, confirmed the biocompatible characteristics that resulted in the preservation of the pulp.
Clinical case
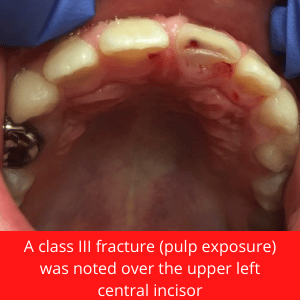
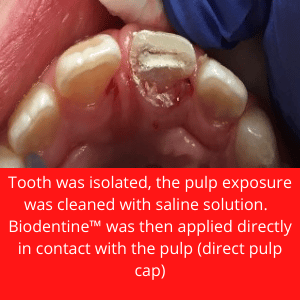
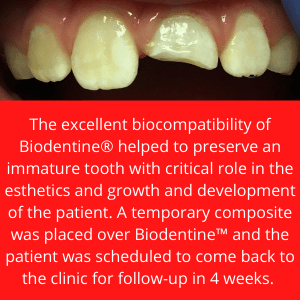
An 8-year-old patient presented to our hospital dental clinic after trauma of the front teeth. She was practicing gymnastics and fell off the monkey bars approximately 1 hour before coming to the hospital.
Dental decay: An overview
Dental decay is the most common chronic childhood disease. Worldwide, 42% of children between the ages of 2 to 11 years old have dental caries in the primary dentition. Premature primary or permanent tooth loss can be caused by dental caries and infection, trauma, or ectopic eruption of permanent teeth, however dental decay is the most prominent cause especially for primary and permanent molars. Poor dietary habits, poor oral hygiene habits, and low socioeconomic status have been shown to be correlated with higher caries incidence and premature tooth loss. Following dental decay as the most common cause of premature loss of primary and permanent teeth is trauma.
Risks of premature tooth loss
Keeping immature (and mature) teeth in the oral cavity is critical for many reasons. Let’s review some of the reasons. Pediatric oral health care has several special considerations within the treatment planning process, including children’s growth and development. Maintenance of arch integrity as children transition from primary to mixed dentition is essential to the development of permanent dentition. The primary dentition has several purposes. Not only does it allow for mastication for adequate nutrition, proper occlusion and esthetics, but they affect the development of speech in children. When lost prematurely, there can be negative consequences seen in the psychological and emotional well-being of children and adolescents. Tooth loss can be considered premature when primary teeth are extracted prior to the normal exfoliation timing. Another major consequence of premature loss of primary teeth is space loss in the permanent arch, as well as crowding and malocclusion. Specifically, the premature loss of primary molars has been found to be associated with major malalignment of the permanent teeth. These effects on succedaneous teeth can result in more expensive and extensive treatment needs in the future.
How to evaluate space maintenance?
Premature tooth loss can lead to space loss but there are several factors to consider when deciding to implement space maintenance for patients in primary and mixed dentition. Specific criteria to consider when evaluating the need for space maintenance includes:
✓ The time that has passed since tooth loss
✓ The chronological age of the child, the dental age or development of the child
✓ Amount of space closure already observed, where in the arch tooth loss is observed
✓ Direction of space closure
✓ The timing of eruption of the succedaneous teeth
✓ The amount of bone remaining over the unerupted permanent tooth.
Premature loss of primary molars poses a significant risk for space loss in the dental arch, making patients three times more likely to require orthodontic treatment after reaching complete permanent dentition. Premature loss of primary anterior teeth does not pose the same risk for space loss in the dental arch. However, premature loss of immature permanent maxillary teeth has deep impact in the esthetics and self-esteem of the patient.
Preserving pulp in traumatized teeth
The occurrence of trauma in the permanent immature teeth is common worldwide. Two thirds of all dental trauma have been reported to occur in children and adolescents with the anterior permanent teeth being the most affected. Traumatic injuries may result in pulp exposure, which may lead to infection. Complicated crown fractures in immature teeth presents a special challenge for the dentist. The main idea is to preserve the pulp inside the root to allow the tooth to complete the root formation and the apex closure. The main objective when preserving the pulp is the use a highly biocompatible material. A favorable material will ensure long term survival of the tooth and avoid the extraction. Various dental materials have advocated for use in direct contact with the pulp.
Traumatized teeth management with Biomaterials
Biodentine™ has excellent properties that protect the vitality of the traumatized tooth pulp:
✓ The setting time, which is around 9-12 minutes. There is a significant difference in the setting time compared with other similar cements (like MTA).
✓ The compression strength of Biodentine™ is similar to the dentin. The use of etch over Biodentine™ does not affect the compressive strength of the material.
✓ The porosity: Because of the low content of water of Biodentine™ the porosity of the material is lower compared with other materials. This is a significant benefit when a perfect seal is mandatory, like in direct pulp cap treatment.
✓ The radiopacity, thanks to the content of zirconium is ideal and allows the practitioner to visualize the material on the radiographs.
✓ The antibacterial property is attributed to the high pH of the material. The high alkalinity has inhibitory effect on the growth of microorganisms.
✓ The biocompatibility of Biodentine™ is outstanding and has been probed in multiple studies when the material is placed with fibroblasts from the pulp.
Preserving immature primary and permanent teeth is a critical task of contemporary dentistry. Placing a dental material in direct or indirect contact with the pulp is a common option that the dentist has in the treatment armamentarium to guarantee the preservation of the pulp tissue. Biodentine™, as described above, is highly biocompatible. This ability was investigated in multiple studies in the past 5 years. Biodentine™, when applied to human pulp cells, confirmed the biocompatible characteristics that resulted in the preservation of the pulp.
Clinical case
An 8-year-old patient presented to our hospital dental clinic after trauma of the front teeth. She was practicing gymnastics and fell off the monkey bars approximately 1 hour before coming to the hospital.
Dental decay: An overview
Dental decay is the most common chronic childhood disease. Worldwide, 42% of children between the ages of 2 to 11 years old have dental caries in the primary dentition. Premature primary or permanent tooth loss can be caused by dental caries and infection, trauma, or ectopic eruption of permanent teeth, however dental decay is the most prominent cause especially for primary and permanent molars. Poor dietary habits, poor oral hygiene habits, and low socioeconomic status have been shown to be correlated with higher caries incidence and premature tooth loss. Following dental decay as the most common cause of premature loss of primary and permanent teeth is trauma.
Risks of premature tooth loss
Keeping immature (and mature) teeth in the oral cavity is critical for many reasons. Let’s review some of the reasons. Pediatric oral health care has several special considerations within the treatment planning process, including children’s growth and development. Maintenance of arch integrity as children transition from primary to mixed dentition is essential to the development of permanent dentition. The primary dentition has several purposes. Not only does it allow for mastication for adequate nutrition, proper occlusion and esthetics, but they affect the development of speech in children. When lost prematurely, there can be negative consequences seen in the psychological and emotional well-being of children and adolescents. Tooth loss can be considered premature when primary teeth are extracted prior to the normal exfoliation timing. Another major consequence of premature loss of primary teeth is space loss in the permanent arch, as well as crowding and malocclusion. Specifically, the premature loss of primary molars has been found to be associated with major malalignment of the permanent teeth. These effects on succedaneous teeth can result in more expensive and extensive treatment needs in the future.
How to evaluate space maintenance?
Premature tooth loss can lead to space loss but there are several factors to consider when deciding to implement space maintenance for patients in primary and mixed dentition. Specific criteria to consider when evaluating the need for space maintenance includes:
✓ The time that has passed since tooth loss
✓ The chronological age of the child, the dental age or development of the child
✓ Amount of space closure already observed, where in the arch tooth loss is observed
✓ Direction of space closure
✓ The timing of eruption of the succedaneous teeth
✓ The amount of bone remaining over the unerupted permanent tooth.
Premature loss of primary molars poses a significant risk for space loss in the dental arch, making patients three times more likely to require orthodontic treatment after reaching complete permanent dentition. Premature loss of primary anterior teeth does not pose the same risk for space loss in the dental arch. However, premature loss of immature permanent maxillary teeth has deep impact in the esthetics and self-esteem of the patient.
Preserving pulp in traumatized teeth
The occurrence of trauma in the permanent immature teeth is common worldwide. Two thirds of all dental trauma have been reported to occur in children and adolescents with the anterior permanent teeth being the most affected. Traumatic injuries may result in pulp exposure, which may lead to infection. Complicated crown fractures in immature teeth presents a special challenge for the dentist. The main idea is to preserve the pulp inside the root to allow the tooth to complete the root formation and the apex closure. The main objective when preserving the pulp is the use a highly biocompatible material. A favorable material will ensure long term survival of the tooth and avoid the extraction. Various dental materials have advocated for use in direct contact with the pulp.
Traumatized teeth management with Biomaterials
Biodentine™ has excellent properties that protect the vitality of the traumatized tooth pulp:
✓ The setting time, which is around 9-12 minutes. There is a significant difference in the setting time compared with other similar cements (like MTA).
✓ The compression strength of Biodentine™ is similar to the dentin. The use of etch over Biodentine™ does not affect the compressive strength of the material.
✓ The porosity: Because of the low content of water of Biodentine™ the porosity of the material is lower compared with other materials. This is a significant benefit when a perfect seal is mandatory, like in direct pulp cap treatment.
✓ The radiopacity, thanks to the content of zirconium is ideal and allows the practitioner to visualize the material on the radiographs.
✓ The antibacterial property is attributed to the high pH of the material. The high alkalinity has inhibitory effect on the growth of microorganisms.
✓ The biocompatibility of Biodentine™ is outstanding and has been probed in multiple studies when the material is placed with fibroblasts from the pulp.
Preserving immature primary and permanent teeth is a critical task of contemporary dentistry. Placing a dental material in direct or indirect contact with the pulp is a common option that the dentist has in the treatment armamentarium to guarantee the preservation of the pulp tissue. Biodentine™, as described above, is highly biocompatible. This ability was investigated in multiple studies in the past 5 years. Biodentine™, when applied to human pulp cells, confirmed the biocompatible characteristics that resulted in the preservation of the pulp.
Clinical case
An 8-year-old patient presented to our hospital dental clinic after trauma of the front teeth. She was practicing gymnastics and fell off the monkey bars approximately 1 hour before coming to the hospital.